|
7/26/2023 0 Comments Lumen ohm graphThe mechanisms of autoregulation in the brain are not completely understood and likely differ with increases vs. At this point, clinical signs of hypoperfusion occur, including dizziness, altered mental status, and eventually irreversible tissue damage (infarction). Clinical signs or symptoms of ischemia are not seen until the decrease in perfusion exceeds the ability of increased oxygen extraction to meet metabolic needs. The reduction in cerebral blood flow is compensated for by an increase in oxygen extraction from the blood. When CPP falls below the lower limit of autoregulation, cerebral ischemia ensues. Above and below this limit, autoregulation is lost and cerebral blood flow becomes dependent on mean arterial pressure in a linear fashion. 
In normotensive adults, cerebral blood flow is maintained at ~50 mL per 100 g of brain tissue per minute, provided CPP is in the range of ~60 to 160 mmHg. Autoregulation is present in many vascular beds, but is particularly well-developed in the brain, likely due to the need for a constant blood supply and water homeostasis. Īutoregulation of cerebral blood flow is the ability of the brain to maintain relatively constant blood flow despite changes in perfusion pressure. Thus, radius is the most powerful determinant of blood flow and even small changes in lumen diameter have significant effects on cerebral blood flow, and it is by this mechanism that vascular resistance can change rapidly to alter regional and global cerebral blood flow. Blood flow is also estimated by Poiseuielle’s law that states that flow is directly related to Δ P, blood viscosity, and the length of the vessel (assumed to be constant) and inversely related to radius to the fourth power: flow = (8 × η × L)/ r 4. Therefore, Δ P is calculated as the difference in CPP and either venous pressure or ICP, whichever is greater. Venous pressure is normally low (2–5 mmHg) and is influenced directly by intracranial pressure (ICP). 
In the brain, Δ P is cerebral perfusion pressure (CPP), the difference between intra-arterial pressure and the pressure in veins. Ohm’s law states that flow is proportional to the difference in inflow and outflow pressure (Δ P) divided by the resistance to flow ( R): flow = Δ P/ R. These assumptions do not apply to large arteries that have thick walls or in the microcirculation in which flow is non-Newtonian. Therefore, coordinated flow responses occur in the brain, likely due to conducted or flow-mediated vasodilation from distal to proximal arterial segments and to myogenic mechanisms that increase flow in response to decreased pressure (see Myogenic Response).īrain blood flow can be modeled from a physical standpoint as flow in a tube with the assumptions that flow is steady, laminar, and uniform through thinned-walled (the wall is <10% of the lumen) non-distensible tubes. However, in order for flow to increase to areas within the brain that demand it, upstream vessels must dilate in order to avoid reductions in downstream microvascular pressure. The high metabolic demand of neuronal tissue requires tight coordination between neuronal activity and blood flow within the brain parenchyma, known as functional hyperemia (see Neural–Astrocyte Regulation).  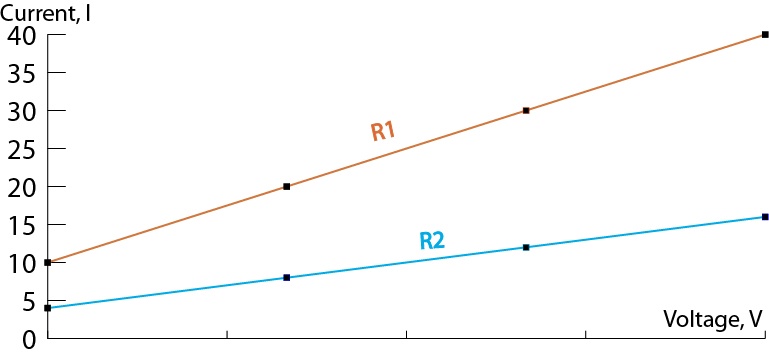
In addition, parenchymal arterioles have considerable basal tone and also contribute significantly to vascular resistance in the brain. In a normal physiological state, total blood flow to the brain is remarkably constant due in part to the prominent contribution of large arteries to vascular resistance (see Segmental Vascular Resistance). The brain uses ~20% of available oxygen for normal function, making tight regulation of blood flow and oxygen delivery critical for survival.
0 Comments
Leave a Reply. |
 RSS Feed
RSS Feed
